Hamilton Spectator
July 18/19 by Joanna Frketich

Hamilton Health Team Co-Chairs John Fleming and Bernice King
Hamilton and Burlington organizations want to be among the first to adopt a major overhaul of the health care system by the Progressive Conservative government.
Health and social service agencies have banded together in each city to put forth separate applications to create Ontario Health Teams (OHT), which are expected to oversee dramatic changes in how local care is provided.
Both proposals got the go-ahead Thursday to move to the next stage in the application process to form the first OHTs in the province.
“I don’t think anybody at the table is sitting there because they think the whole thing is broken,” said Paul Johnson, who is representing the city in Hamilton’s proposed health team. “They are sitting at the table because they see such opportunity.”
The legislation for the health system revamp came into effect June 6 under the Connecting Care Act. An investigative series Operation Health Care Reform by The St. Catharines Standard and The Hamilton Spectator starting Saturday (July 20) will provide the most comprehensive coverage to date of the overhaul considered the biggest change since Medicare.
The plan announced in February puts a super agency named Ontario Health in charge of the entire health care system — from hospitals to community care to organ donation to cancer care. The super agency will oversee dozens of regional teams made up primarily of health and social service organizations working together to integrate services locally and help area residents navigate the system.
The Ministry of Health got over 150 OHT applications in May provincewide despite few details being known about how the teams will be governed, funded or operate. The province has said, OHTs will evolve over time based on the experiences of the initial groups.
“This could be the biggest transformation we’ve seen certainly in a long time,” said Johnson. “If we work differently, we can really change the outcomes in terms of better care.”
The Hamilton application is made up of 18 health and social services agencies including Hamilton Health Sciences, St. Joseph’s Healthcare, McMaster University and the city. But there is room for more to join.
“Our principle really is there is an open chair,” said Johnson. “I don’t think any of us are convinced the table is full.”
What makes the Hamilton bid particularly unique is that it is chaired by former cancer patients John Fleming and Bernice King.
“I haven’t been part of too many processes where we really have embedded a patient experience right from the beginning,” said Johnson. “Normally we would get through these first applications and say, ‘You know we really need to find some patients.’ Of course, we’ve decided what we’re doing long before.”
For Hamilton’s OHT application, patients are at the forefront of mapping out a new local health care system.
“It was an opportunity I couldn’t pass up,” said King, who was treated for lung and gynecological cancer.
Both King and Fleming feel this is a chance to give back to the system that helped them when they needed it most and improve it for the next patients.
“I’m here partly because this city and all of its health care systems saved my life literally,” said Fleming who was treated for melanoma. “I’m 100 per cent on board with what is going on and I want to contribute and I want to help.”
He describes their job as being “the relentless conscience of this project to never lose sight of keeping patients at the centre of this.”
The Burlington group also put patients first when it decided to make family medicine the focus of its application with all but two of the eight organizations being primary care providers.
“Our team recognizes the importance of primary care as the foundation of the health care system and that’s why I agreed to sign up for it,” said family physician Dr. Harpal Singh, who is the co-chair of the proposed Burlington OHT. “We feel this kind of model really should be the model of care throughout Ontario.”
So far the proposed Burlington team accounts for 60,000 rostered patients but it’s also hoping to grow.
“We’re still trying to get the word out to physicians in Burlington,” said Singh, lead doctor at the North Burlington Medical Centre Family Health Group. “Due to privacy laws we’re not even allowed to have access to physicians’ emails without their permission. These are the kinds of barriers that inhibit care for patients.”
Teams being considered to form the first OHTs have been asked to put in a full application to represent a geographic area with a population up to 500,000. The early adopters will be announced in the fall.
Both Hamilton and Burlington groups are confident they will be among the first OHTs because health and social service organizations have long collaborated in this area.
“Why I think we’re a bit optimistic is that we’ve put the work in prior to this,” said Johnson. “This really builds on work that’s been going on in Hamilton. We’ve been thinking about what health care means in the broadest sense of that term from the social determinants of health umbrella.”
One of the reasons Hamilton is so far ahead is an ongoing project started in 2010 by The Spectator called Code Red that found glaring disparities between neighbourhoods in Hamilton including a 21-year difference in average age at death. It long ago helped foster ongoing collaboration between health and social service agencies.
Johnson gives the example of the patient with chronic obstructive pulmonary disease who ends up in the emergency room four to five times every summer because the progressive lung disease is exacerbated by heat.
“This primary care physician is saying it would be great if they had an air conditioner and I say we have a program that could deliver an air conditioner,” said Johnson. “Those are the little things.”
The OHTs will aim to bridge the gaps that often leave patients lost by having multiple providers band together to take joint accountability for the entire journey through the system.
“I often look around and think we have it all here,” said Johnson. “What is holding us back is the inability to do the things we know we need to do. Sometimes that is because we don’t have the relationships with each other to even know someone else could do it. We’re a bit discoordinated.”
Drastically changing how health care providers interact is the only way the system will be able to cope with the growing and aging population, says Singh.
“Healthcare often is relatively insatiable in the amount of expectations that we have,” said Singh. “In order to work with limited resources we need to organize ourselves better.”
Joining the OHT requires a leap of faith considering neither group has come up with a governance structure yet or knows what will happen to their funding when the province provides one envelope of cash per patient to be shared among all the services.
“We’d be naïve to say everybody around the table is not thinking about that,” said Johnson. “When people already have a bit of a relationship — believe me it’s not all kumbaya moments — there is at least that level of trust that we are going to continue to work at this and even if it’s not perfect yet we’ll keep making it better.”
There’s no startup funds so the organizations involved have to find a way to pay for the costs of the application and the administration of the proposed OHT.
“There is no pot of money being offered by Queen’s Park,” said Fleming. “It’s figure out how to put this together within the resources of our team.”
In addition, the OHT has to navigate making sure small organizations in the group get a voice when massive players like HHS, St. Joseph’s and Joseph Brant Hospital are involved.
“There are physicians in Burlington who have felt that the hospital has their agenda and family doctors have their agenda and they don’t necessarily align,” said Singh. “We work in that fragmented and siloed way and it becomes really increasingly difficult for patients to get proper care or to negotiate through that system.”
Both groups say they won’t quit even if they aren’t chosen to be among the first teams.
“Whether we are an early adopter or not, our position has been that we are going ahead at the same pace that we have been to date, this is such important work.” said Dr. Cheryl Williams, co-chair of the proposed Burlington OHT and executive vice president clinical at Joseph Brant.
Her co-chair Singh expects the province to keep working with teams not initially chosen until they are ready to become an OHT in future waves of the roll out.
“Our plan to co-operate, break down barriers and provide the best kind of care for our patients is going to move forward,” he said. “It’s just going to get stronger.”
July 2, 2019 – Canadian Healthcare Technology
HAMILTON, ONT. – St. Joseph’s Health System (SJHS) is using video visits to connect clinicians with discharged surgical patients at home.
The video-based care builds on St. Joseph’s use of one phone-number access to an integrated care team, around the clock, for discharged patients and provides another dimension of support in their homes.
The video service was launched in January of this year, in conjunction with the Ontario Telemedicine Network (OTN), St. Joseph’s Healthcare Hamilton (Hospital) and St. Joseph’s Home Care, and started with patients discharged from thoracic, hip and knee surgeries.
Once at home, the patients can use computers, tablets or smartphones to interact visually and by voice with a coordinator who is able to answer their questions and can connect them with other members of the care team. Virtual “face-to-face” visits can be scheduled with clinicians, home care nurses, and the patients access these visits through a digital patient portal called MyDovetale.
Since 2012, St. Joseph’s has pioneered a new model of care called Integrated Comprehensive Care (ICC), which gives patients and their families access to One Health Team, One Digital Record, and One Number to Call, 24/7.
Patients first meet their ICC coordinator while in hospital, to receive discharge information, learn about the ICC program and support they will receive at home. Once the patient is in the community, the ICC team uses ‘virtual rounds’ to discuss patients and their care plan together.
Everyone is in the loop and patients don’t repeat their information every time.
“We’re the first Hospital in Ontario to use integrated virtual care software, outside of the Ontario Telemedicine Network OTNhub, to support our patients,” said Andriana Lukich, program manager.
The video service is integrated with the hospital’s new Epic information system (branded as Dovetale), so that clinical records, including diagnostic images and lab test results, can be pulled up and shared while the meeting is going on.
Clinicians can write notes and update the records while they’re conducting the video encounters. The proof of concept is now being expanded to new patient populations at St Joseph’s and has paved the way for OTN’s new Partner Video Project initiative, Lukich said.
The pilot project discovered that virtual visits are not for everyone. Some patients struggled with the technology, and small factors like lighting and avoiding the mute key on a phone could hinder interactions with clinicians.
For that reason, the standard telephone is available for all patients – it’s still the easiest way to reach the ICC team, any time night or day.
Secure Messaging through the MyDovetale patient portal is also offered.
Lukich and hospital Chief Information Officer Tara Coxon discussed St. Joseph’s virtual care solution at the Technology & the Future of Healthcare conference, held in Hamilton in May.
The ICC program has been further enabled by St. Joseph’s Healthcare Hamilton’s implementation of Epic (Dovetale), which went live at St. Joseph’s in December 2017. At that time, said Coxon, St. Joe’s became a digital hospital and jumped to HIMSS EMRAM Stage 6. “Previous to that, we were at EMRAM 1.2,” she said. “It was an over-night transformation.”
The Epic implementation at St. Joseph’s Healthcare Hamilton was named Dovetale to signify the joining of technology with compassion. The system is helping to smooth out some of the pain points in Ontario’s healthcare system, specifically the hand-offs that occur when patients move from one level of care to another.
In one recent instance, a lung cancer patient who underwent surgery at St. Joseph’s was discharged home to Beamsville, only to discover that his wound seemed abnormal. He was worried it might have become infected.
He contacted his ICC coordinator at St. Joseph’s using the one-number service, and she instigated an ad hoc video visit to view the wound in real-time and determined that the patient should receive care right way.
This was arranged through St. Joseph’s Home Care, and on the same day, a visiting nurse travelled to the patient’s home and changed his wound dressings. She also updated his chart, right on the spot.
St. Joseph’s is making medical records available to the patients themselves through the use of a portal – called MyDovetale. “We were hearing that patients wanted better access to their records and that they wanted their records to be accurate and accessible throughout the system,” said Lukich.
In the summer of 2018, St. Joseph’s went live with the MyDovetale portal, extending it to patients in the mood disorder and kidney transplant clinics.
Patients can access their records on any platform, but it’s been found that smartphones are now the most popular device. Access can be given to family members, loved ones and members of care teams. Lukich said that 88 percent of patients report that MyDovetale has allowed them to take better care of themselves. Meanwhile, the video visit service has saved some patients two to three hours of travel time.
Patients have been asking for enhancements to the MyDovetale solution – in particular, they’d like to see prescription renewals and diagnostic imaging reports made available on the system.
MyDovetale will soon be rolled out to 80,000 more patients – an organization-wide rollout.
According to St. Joseph’s, the ICC program has resulted in a savings of up to $4,000 per patient, a 30 percent reduction in emergency department visits and 30 percent reduction in hospital readmissions with a 98 percent patient satisfaction approval rating. It’s doing this by enabling patients to stay comfortably in their homes, getting the reassurance or care they need without visiting the hospital.
The program has been so successful that Ontario’s health ministry would like to expand it to other healthcare providers.
“Already, St. Joseph’s has coached over 30 other organizations on how they might implement an ICC model of their own,” commented Fraser Edward, VP partnerships at SJHS.
“We have established the Centre for Integrated Care to help support Ontario Health Teams and other healthcare providers wrap physical and virtual care around the needs of patients and their families.” For more information, see: www.sjhs.ca/integratedcare/cic/
St. Joseph’s Health System’s pioneering Integrated Comprehensive Care model for COPD/CHF patients could free up 13,502 hospital days annually across the province: Health System Performance Research Network (HSPRN)
June 27, 2019 – Hamilton, ON – A program pioneered by St. Joseph’s Healthcare Hamilton and St. Joseph’s Home Care, members of St. Joseph’s Health System (SJHS), has the potential to free up more than 13,000 hospitals days and save $24.1M in health care if it were spread across the province, according to a new research report.
Conducted by University of Toronto-affiliated Health System Performance Research Network (HSPRN) the evaluation analyzes six existing healthcare programs in Ontario with the aim of creating seamless transitions from hospital to home care. This is done by integrating care for patients through one team, one number to call 24/7 and one electronic record to support their care and save healthcare dollars – the key principles outlined in the government’s vision for Ontario Health Teams
St. Joseph’s Health System pioneered this model of care when it developed Integrated Comprehensive Care (ICC) in 2012. The MOHLTC later expanded the model to other sites throughout the Province, and SJHS partnered to expand ICC across 12 acute centres in the Hamilton Niagara Haldimand Brant (HNHB) Local Health Integration Network (LHIN) for all Chronic Obstructive Pulmonary Disease (COPD) and Congestive Heart Failure (CHF) patients. SJHS was also brought on board by the MOHLTC to support the provincial roll out. The HSPRN report evaluates this expansion.
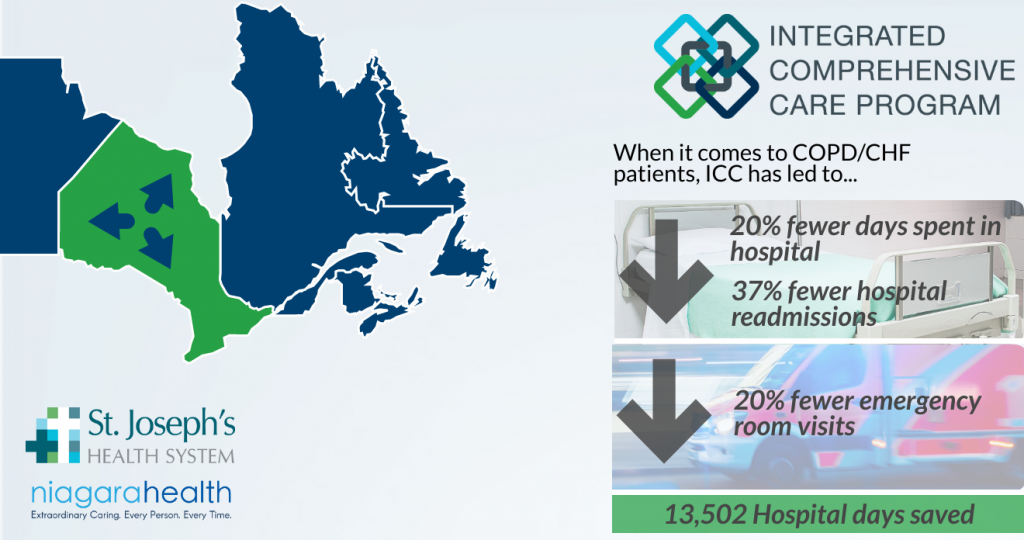
The evaluation found that all six programs are having a positive effect on reducing hallway medicine. In particular, the total number of days patients spent in the hospital was reduced by more than 20%, readmissions were also reduced up to 37%, and there was an overall 20% relative reduction in Emergency Department visits. In addition, the report highlights that if the SJHS’ COPD/CHF ICC model was spread provincially to all 18,538 patients in Ontario, estimated annual savings of 13,502 hospital days and $24.1M dollars could be achieved.
“I was surprised at how successful HNHB ICC was at improving the transition of care for people with complex medical conditions,” says Walter Wodchis, Principal Investigator of the report and a Professor at the University of Toronto. “The collaboration they built between hospital and post-acute providers was crucial. I don’t think there has been another program that’s been quite [this] successful internationally.”
“This program was created by a group of nurses, PSW’s and frontline workers from the bottom up,” says Danielle Fox, St. Joseph’s Home Care Nurse. “We were given autonomy and flexibility to do what we needed to provide care to the patients. The one team approach and our focus around continuity of care, building rapport and educating caregivers/families as part of the care team are the keys to its success.”
The report recommends the MOHLTC implement a similar model of care for surgical procedures. Earlier this year, St. Joseph’s Healthcare Hamilton and Niagara Health announced they would be one of the first acute hospitals in Ontario to provide ICC program to all planned surgical patients with virtual care options by the end of 2019.
“The results speak for themselves,” says Dr. Thomas Stewart, President & CEO of St. Joseph’s Health System and CEO of Niagara Health. “We’re breaking down silos and working together with primary care and community partners. By coordinating our patient’s care from hospital to home, we not only see favourable outcomes for our patient’s and caregiver’s health, physically and mentally, but we are contributing to ending hallway medicine by freeing up much-needed beds and resources. It’s a win-win.”
ICC Patient/Caregiver testimonials:
• “It’s a marvellous thing. If there’s any chance that I can continue the program, I would jump at the chance. This team is the best, and I have never had anything like it.”
• “It was excellent. All the people that were involved were great. I wish that I’d known about it sooner.”
• “The ICC program has been an excellent help for me and my husband. It was comforting to know there was someone I could call for answers to any health concerns that might arise. The nurses, physiotherapist and dietitian, were all most pleasant and provided much valuable information to best help my husband, and therefore, me!!”
Quick Facts:
• St. Joseph’s Health System pioneered Integrated Comprehensive Care (ICC) and was the first healthcare initiative in Ontario to show the benefits of an Integrated Care approach between the hospital and the community. To learn more about the ICC Program: https://sjhs.ca/integratedcare/
• St. Joseph’s Home Care is the lead Home Care Agency for the HNHB ICC program. Nurses, PSW’s, Physiotherapists and other frontline staff are educated on caring for specific patient streams within the ICC program. To learn more about St. Joseph’s Home Care: https://www.stjosephshomecare.ca/
• Niagara Health, serving over 450,000 residents, contributes to the highest proportion of patients in the COPD/CHF program across HNHB. To learn more about Niagara Health: https://www.niagarahealth.on.ca/
Project partners:
HNHB Community Care Access Centre, HNHB Local Health Integration Network, HNHB Primary Care lead, Brant Community Healthcare System, Centre de Santé Communautaire, Grand River Community Health Centre, Haldimand War Memorial Hospital, Hamilton Health Sciences, Joseph Brant Hospital, Niagara Falls Community Health Centre, Niagara Health, Norfolk General Hospital, North Hamilton Community Health Centre, ProResp, SE Health, St. Joseph’s Healthcare Hamilton, St. Joseph’s Home Care, VitalAire, West Haldimand General Hospital
About St. Joseph’s Health System
St. Joseph’s Health System is one of the largest healthcare organizations in Canada, and only system in Ontario delivering a full continuum of health care services. Medical and specialty services affect care at all points and include acute care, long-term care, home care, hospice and research & education. SJHS is a globally recognized leader for innovation in models of patient-centred integrated care. St. Joseph’s Health System has a unique partnership with Niagara Health to leverage each organization’s strengths to bring better care to the people in the communities we serve.
About Niagara Health
Niagara Health (NH) is a community-based academic centre with a focus on teaching and learning, research and innovation. We are very proud of our strong partnership with the St. Joseph’s Health System and our academic partners including McMaster University, Brock University and Niagara College. Serving more than 450,000 residents across 12 municipalities making up the Regional Municipality of Niagara, NH is a regional healthcare provider with multiple sites and a growing network of community-based services. The team is made up of more than 4,800 employees, 600 physicians, and 850 volunteers to deliver ‘Extraordinary Caring. Every Person. Every Time’. We provide a wide range of inpatient and outpatient services to residents across Niagara, including Acute Care, Cancer Care, Cardiac Care, Complex Care, Emergency and Urgent Care, Kidney Care, Mental Health and Addictions, Stroke Care, Surgical Care and Long-Term Care.

