St. Joseph’s says use of virtual visit tech has increased 450 per cent
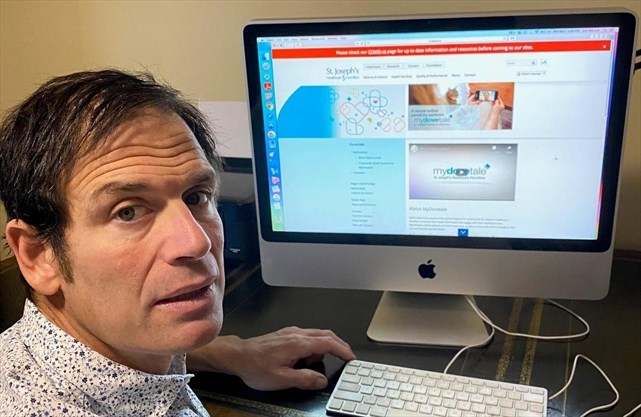
Rob DeLuca, a bodybuilder with stage-four lung cancer and pulmonary hypertension, uses St. Joseph’s Healthcare Hamilton’s digital patient portal, MyDovetale, from his Ancaster home.
Apr 01, 2020 by Sebastian Bron Hamilton Spectator
For Rob DeLuca, an ordinary trip to the doctor’s office often feels like tiptoeing through a room filled with trip wires.
The bodybuilder with stage-four lung cancer and pulmonary hypertension is acutely vulnerable to commonly transmitted germs. Touchscreen parking posts, arm rests on chairs, door handles, washrooms: they’re all akin to booby traps that could trigger an infection and kick his immune system into overdrive.
But that’s changed as the outbreak of COVID-19 has forced health-care providers to embrace physical distancing and modify their outpatient care services.
DeLuca was one of more than 1,000 at-risk St. Joseph’s Healthcare Hamilton (SJHH) patients to have received virtual care in March, chatting with doctors and getting condition updates from the comfort of their own homes.
“It’s made a big difference, especially since we’ve always had to be ultra-mindful when going to the doctor and now that’s been (amplified) with the virus,” said DeLuca, who meets with a respirologist every three months.
“There’s no travel, getting through several doors, touching many surfaces. There’s more time to discuss with (the doctor) and my wife can sit comfortably on the couch taking detailed notes.”
SJHH has seen an approximately 450 per cent increase in virtual-care volume since its personalized, digital patient portal, MyDovetale, was streamlined last month to cope with the number of people who wouldn’t be able to access on-site services.
Tara Coxon, chief information officer, said SJHH has seen an increase from 100 patients before the crisis — most of them mental health — to about 5,000 now across 19 clinics.
“Emergency visits to clinics are still operating, but for the part we’ve had every service go digital,” she said.
The user-friendly system has given doctors a reliable means of adapting their care to the current limits of the health crisis. For patients whose technical capacity is underdeveloped, like seniors, the health centre has a team of nurses and researches help get them on board.
“Physical distancing is critically important during COVID-19, and this has helped us go on with business as usual,” said Dr. Nathan Hambly, a respirologist at SJHH’s Firestone Clinic and DeLuca’s doctor.
The Firestone Clinic has about 700 patients with complex respiratory diseases, a majority of which boast survival rates of around three to five years.
With appointments typically scheduled months ahead of time, Hamby said the virtual portal — and in particular seeing his patients over a screen — has proven imperative in offering patients consistent, accurate care during the health crisis.
“One might say that a telephone would be just as good in these situations, but it isn’t. By looking at a patient, you’re able to ask questions and see their breathing and how hard it is for them to breath in real time,” he said.
Sebastian Bron is a Hamilton-based reporter at the Spectator. Reach him via email: sbron@thespec.com
July 2, 2019 – Canadian Healthcare Technology
HAMILTON, ONT. – St. Joseph’s Health System (SJHS) is using video visits to connect clinicians with discharged surgical patients at home.
The video-based care builds on St. Joseph’s use of one phone-number access to an integrated care team, around the clock, for discharged patients and provides another dimension of support in their homes.
The video service was launched in January of this year, in conjunction with the Ontario Telemedicine Network (OTN), St. Joseph’s Healthcare Hamilton (Hospital) and St. Joseph’s Home Care, and started with patients discharged from thoracic, hip and knee surgeries.
Once at home, the patients can use computers, tablets or smartphones to interact visually and by voice with a coordinator who is able to answer their questions and can connect them with other members of the care team. Virtual “face-to-face” visits can be scheduled with clinicians, home care nurses, and the patients access these visits through a digital patient portal called MyDovetale.
Since 2012, St. Joseph’s has pioneered a new model of care called Integrated Comprehensive Care (ICC), which gives patients and their families access to One Health Team, One Digital Record, and One Number to Call, 24/7.
Patients first meet their ICC coordinator while in hospital, to receive discharge information, learn about the ICC program and support they will receive at home. Once the patient is in the community, the ICC team uses ‘virtual rounds’ to discuss patients and their care plan together.
Everyone is in the loop and patients don’t repeat their information every time.
“We’re the first Hospital in Ontario to use integrated virtual care software, outside of the Ontario Telemedicine Network OTNhub, to support our patients,” said Andriana Lukich, program manager.
The video service is integrated with the hospital’s new Epic information system (branded as Dovetale), so that clinical records, including diagnostic images and lab test results, can be pulled up and shared while the meeting is going on.
Clinicians can write notes and update the records while they’re conducting the video encounters. The proof of concept is now being expanded to new patient populations at St Joseph’s and has paved the way for OTN’s new Partner Video Project initiative, Lukich said.
The pilot project discovered that virtual visits are not for everyone. Some patients struggled with the technology, and small factors like lighting and avoiding the mute key on a phone could hinder interactions with clinicians.
For that reason, the standard telephone is available for all patients – it’s still the easiest way to reach the ICC team, any time night or day.
Secure Messaging through the MyDovetale patient portal is also offered.
Lukich and hospital Chief Information Officer Tara Coxon discussed St. Joseph’s virtual care solution at the Technology & the Future of Healthcare conference, held in Hamilton in May.
The ICC program has been further enabled by St. Joseph’s Healthcare Hamilton’s implementation of Epic (Dovetale), which went live at St. Joseph’s in December 2017. At that time, said Coxon, St. Joe’s became a digital hospital and jumped to HIMSS EMRAM Stage 6. “Previous to that, we were at EMRAM 1.2,” she said. “It was an over-night transformation.”
The Epic implementation at St. Joseph’s Healthcare Hamilton was named Dovetale to signify the joining of technology with compassion. The system is helping to smooth out some of the pain points in Ontario’s healthcare system, specifically the hand-offs that occur when patients move from one level of care to another.
In one recent instance, a lung cancer patient who underwent surgery at St. Joseph’s was discharged home to Beamsville, only to discover that his wound seemed abnormal. He was worried it might have become infected.
He contacted his ICC coordinator at St. Joseph’s using the one-number service, and she instigated an ad hoc video visit to view the wound in real-time and determined that the patient should receive care right way.
This was arranged through St. Joseph’s Home Care, and on the same day, a visiting nurse travelled to the patient’s home and changed his wound dressings. She also updated his chart, right on the spot.
St. Joseph’s is making medical records available to the patients themselves through the use of a portal – called MyDovetale. “We were hearing that patients wanted better access to their records and that they wanted their records to be accurate and accessible throughout the system,” said Lukich.
In the summer of 2018, St. Joseph’s went live with the MyDovetale portal, extending it to patients in the mood disorder and kidney transplant clinics.
Patients can access their records on any platform, but it’s been found that smartphones are now the most popular device. Access can be given to family members, loved ones and members of care teams. Lukich said that 88 percent of patients report that MyDovetale has allowed them to take better care of themselves. Meanwhile, the video visit service has saved some patients two to three hours of travel time.
Patients have been asking for enhancements to the MyDovetale solution – in particular, they’d like to see prescription renewals and diagnostic imaging reports made available on the system.
MyDovetale will soon be rolled out to 80,000 more patients – an organization-wide rollout.
According to St. Joseph’s, the ICC program has resulted in a savings of up to $4,000 per patient, a 30 percent reduction in emergency department visits and 30 percent reduction in hospital readmissions with a 98 percent patient satisfaction approval rating. It’s doing this by enabling patients to stay comfortably in their homes, getting the reassurance or care they need without visiting the hospital.
The program has been so successful that Ontario’s health ministry would like to expand it to other healthcare providers.
“Already, St. Joseph’s has coached over 30 other organizations on how they might implement an ICC model of their own,” commented Fraser Edward, VP partnerships at SJHS.
“We have established the Centre for Integrated Care to help support Ontario Health Teams and other healthcare providers wrap physical and virtual care around the needs of patients and their families.” For more information, see: www.sjhs.ca/integratedcare/cic/

