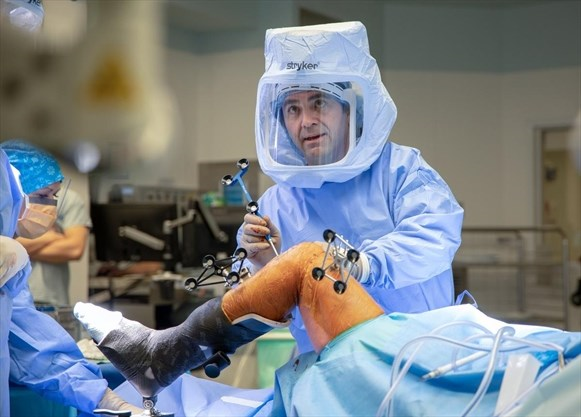
Need a knee replacement? St. Joseph’s Healthcare has a robot that does that
St. Joe’s will do research to prove the technology works to avoid pitfalls plaguing robotic prostate cancer surgery.
Feb 25, 2019, by Joanna Frketich The Hamilton Spectator
Canada’s first knee replacements by a doctor-controlled robot have taken place at St. Joseph’s Healthcare as part of a study to prove the effectiveness of the technology and avoid the ongoing funding pitfalls plaguing prostate cancer surgery.
The robot has been used in four knee operations since Jan 18 in a pilot study funded by hospital donors.
“It’s very fledgling,” said Dr. Anthony Adili, who did the surgeries. “We’re just starting down a very exciting path … At the end of the day I think patients will benefit immensely from this new technology.”
St. Joseph’s, which specializes in robotic surgery, is getting the proof it needs from the start to show the technology is worth the extra cost so it doesn’t end up embroiled in the same dispute it faces with prostate cancer surgery.
“We’re in a golden opportunity to do that kind of pivotal research to inform our decision-making,” said Adili, chief of surgery at St. Joseph’s. “The research is being done (elsewhere) but it’s not high quality research so it’s hard to make definitive decisions and definitely difficult to make policy decisions. We want to produce that high quality data.”
The research is significant because a lack of evidence was behind a controversial recommendation in 2017 by the Ontario Health Technology Advisory Committee (OHTAC) against publicly funding robotic surgery to remove a cancer patient’s prostate gland.
It was a stunning blow to St. Joseph’s, where the vast majority of radical prostatectomies are done with the help of the da Vinci robot system.
Currently, the province pays the hospital the same price as the traditional operation and donors make up the extra cost of the robot. It’s an increasing burden on the St. Joseph’s Healthcare Foundation as the robot is rapidly becoming the surgery of choice with men from Kitchener to Niagara willing to travel and wait longer to get it.
A final decision on whether the province will eventually fund the robot for prostatectomies at an estimated cost of $800,000 — $3.4 million a year has been put off while St. Joseph’s gathers evidence on how it saves the health care system in other ways, such as a faster recovery time, since it’s no longer possible to do randomized trials.
“It’s so ubiquitous and it’s almost the standard of care,” said Adili. “It’s impossible to randomize someone to robotic prostatectomy versus an open prostatectomy. Nobody will go for it. We lost that opportunity.”
Orthopedic robotic surgery was approved in Canada and the United States only in the last year so high-quality studies can still be done. It’s the same for robotic thoracic cancer surgery with St. Joseph’s already running a multicentre trial.
“We don’t know who it’s going to benefit so we can do these randomized trials and develop that data that will help drive decision-making,” said Adili.
The biggest roadblock is that St. Joseph’s is the only centre in Canada doing robotic orthopedic surgery, making a multi-site trial of thousands of patients impossible to do here. With a price tag of $2 million a robot, it will be hard to find other centres with the appetite to join in.
“We’re going to have to partner with centres in the United States and convince them to contribute data,” said Adili. “The problem is they are buying robots like crazy because it is driving their business. They are going to be less inclined to want to randomize one versus the other. Some of our progress will be hampered until we get more units in Canada because Canadians have a very different mindset and will participate in trials.”
In the meantime, St. Joseph’s has started the pilot study that it hopes will provide enough evidence to get grants for the eventual large trial.
It’s important because Adili says one in five patients are currently unhappy with the outcome of their knee replacement and the robot’s precision could drop that number substantially. In addition, it makes partial knee replacements much easier, so surgeons will be more likely to do them.
“By replacing just the bad part of the knee, I’m leaving more of the patient’s normal anatomy behind,” said Adili. “It should feel like a more normal knee, recovery should be quicker and they should have better functionality. A total knee, although it is a successful procedure, it still does not match the mechanics of a normal knee.”
With the popularity of the robot for prostate cancer, Adili doesn’t expect any difficulty in recruiting patients.
The first was 66-year-old Peter Sporta from Oakville, who waited an extra two months to get a robotic partial knee replacement on Jan. 18.
“I wasn’t scared at all” Sporta said about being the first patient. “I couldn’t wait.”
Sporta was in the hospital for one night and walking the next day.
“Within three days I threw away my crunches and my cane,” he said. “For sure I would recommend this.”
By Jim Rankin Toronto Star Reporter | Sun., Dec. 23, 2018
HAMILTON—Think virtual reality and you might picture a fantasy world to be explored and enjoyed. But researchers and staff at a Hamilton hospital are using the technology to better understand what it feels like to be in a seclusion room, the health-care equivalent of a jail segregation cell.
“We wanted to see what it was like to be on the other side of the door,” said Gary Chaimowitz, head of the forensic psychiatry program at St. Joseph’s Healthcare and a professor at McMaster University. “I think many of us can imagine, or recall times when you’ve been in places by yourself, when you didn’t want to be by yourself, left alone, but this puts you, as a staff person, in our rooms.”
Using a VR headset and hand controllers, staff are transported into a room modelled after real seclusion rooms at the hospital, and another set in a jail cell.
SimWave, an Ottawa-based company, used photographs to recreate the experience.
In two of three VR training modules being used at the program, you try to get the attention of virtual staff on the other side of the door. The seclusion room has no bathroom, and your bladder is full. You can ask for help, pace the room and knock or even pound on the door.
Your call for help returns one of 10 programmed responses, ranging from, a polite, “Yes, we’ll get you something,” to “Hold on a sec, we’re a little bit busy right now,” to a little more pointed response, Chaimowitz said.
“The tone, if you’re on the receiving end of that, obviously it makes a hell of a big difference,” he said.
Sometimes, there is no response, or the “patient” hears laughter. In another scenario, you actually get to use the bathroom.
“We’re looking at how long you can be in there before you get anxious,” Chaimowitz said, “and what it’s like to have a different staff response, the idea being that we are going to try to sensitize staff to what it’s like to be on the inside, which might change the way they interact with patients, both in terms of their tone and also a recognition of what it’s like to be there.”
Some staff have had to remove the headset after a while because they feel so enclosed by being in the room, Chaimowitz said, adding no one has found the experience to feel fake. “People have acknowledged that this is very different than being on the other side of the door,” he said.
The artists and developers at SimWave paid close attention to the finest of details. “If you press your virtual nose against the walls you can really see the details,” said Matt Thomas, SimWave’s head of business development.
Many of the hospital’s patients come from jails and return after treatment. Chaimowitz said the hospital hopes to share this training experience with provincial and federal corrections systems, where the use of segregation is under intense scrutiny.
In federal and provincial jails, inmates are being held in segregation for great lengths of time, and often exceeding 15 consecutive days, a point beyond which the United Nations has called to be banned because of the proven psychological harm it can cause.
This fall, as part of a human rights case settlement, Ontario’s Ministry of Community Safety and Correctional Services released two months’ worth of data on inmates either awaiting trial or serving short sentences who had spent time in segregation.
Of 3,998 placements in segregation, 778 were for periods longer than 15 consecutive days, the data revealed.
Half of the inmates had mental health alerts on their files and more than a third had a suicide alert.
“The correctional system is behind,” says Chaimowitz, who gave expert testimony at the coroner’s inquest into the 2007 death of Ashley Smith, who spent more than three years in segregation.
He recalls his first visit, decades ago, to a Hamilton jail. “I could hear people screaming and recognized there were mentally unwell people.”
“I don’t think anybody there is being cruel,” he said. “But it is frightening, and it is one of those sort of things that I can’t believe, in our cities, that we house people like this.”
The VR training can’t replicate everything in a seclusion or segregation setting, such as the degree of noise, the clanging and the smells, but the idea is that “if we can walk in someone’s shoes, even if it’s the way you deal with people, that it will be a little bit more humane,” he said.
Another training module simulates a search for contraband in a psychiatry patient room complete with a full bathroom. A more complex simulation still in the works involves an educational night-shift scenario that begins with hearing a noise and escalates into a hostage-taking situation.
The hospital’s forensic psychiatry unit has 114 beds and will be adding four correctional beds, as part of a pilot project with the provincial ministry that overseas corrections. Those beds should cut down visits by mentally ill inmates to hospital emergency rooms, where staff are “uncomfortable” with corrections patients who are shackled and handcuffed, Chaimowitz said.
“We’ll be in a better position to treat them and get their mental illness under control,” Chaimowitz said. “The idea is to bring them in here and get them well enough” to return to the general jail population, he says. “I think it the potential for making a big difference is very, very high.”
As for more the potential for virtual reality, Chaimowitz and his team would like to see patients given the opportunity to use the technology to escape their rooms and units and explore.
“They are basically stuck in their unit and the perimeter around St. Joe’s and Hamilton. So, they can’t do a lot,” said psychiatrist Sébastien Prat. “We want to develop that kind of project, in order to make them able to travel to a beach or somewhere they want to go, so they can enjoy something.”