
(HAMILTON, NIAGARA) – NOVEMBER 12, 2020 – COVID Care @ Home is a new model of care delivered by St. Joseph’s Home Care (SJHC), in partnership with St. Joseph’s Health System (SJHS), Niagara Health and community partners that connects patients to care wherever they are, whenever they need it.
Starting at St. Joseph’s Healthcare Hamilton and Niagara Health, with rapid expansion to Kitchener, this new model of care for COVID patients will provide 24/7 access to high-quality care from one integrated team in the home and in community settings like retirement homes, shelters and hospices.
COVID Care @ Home is a uniquely designed program intended for those with a confirmed COVID diagnosis who do not require hospitalization. Complimenting existing local COVID initiatives, the program will support integrated care at home, early discharge from hospitals with supports and help to prevent hospitalization. It will also help to prevent outbreaks by providing Infection Prevention and Control (IPAC) and coaching support for community congregate settings.
Patients will be assessed to determine what level of service will be provided. Vulnerable patients who are at risk of hospitalization and who require additional supports and services will have access to an integrated clinical care team, remote monitoring and at-home and virtual visits to support a safe recovery at home. This same model of care will be available to patients discharged from hospital so they can safely return home sooner.
This innovative, flexible model would provide COVID patients access to services that may not typically be within the scope of traditional home and community care supports. Patients will be cared for by one integrated team representing a variety of providers whose clinical decisions are empowered through the use of a single electronic patient record to support patients in the following ways:
- Virtual Care (phone, video and remote patient monitoring)
- One number to call 24/7
- One clinical team
- One electronic record
- System navigation / connection to social supports
- Access to specialists
- IPAC Support
St. Joseph’s Home Care will lead this innovative transformation to connect home care to a broad range of services for COVID patients and work in collaboration with other service provider organizations and primary care.
SJHS is one of the largest healthcare organizations in Canada, and the only system in Ontario delivering a full continuum of integrated health care services.
“We’ve learned a tremendous amount about COVID-19 over the last several months,” said Tom Stewart, St. Joseph’s Health System President and CEO and CEO of Niagara Health. “This new program builds on partnerships and learnings by increasing our focus on virtual care and specialized COVID care teams that crosses normal silos of care. This will help us through the second and future waves of the pandemic as well as prepare us for system transformation needed in healthcare.”
The program is designed to support older adults who are at greater risk of physical and mental health decline. Patients will be enrolled by the clinical teams at the time of their COVID 19 diagnosis.
The new model will also help to protect capacity in hospitals by expanding supports and services in the community through a dedicated team that will facilitate care at home, support safe discharges from hospital and limit unnecessary Emergency Department visits. This will help hospitals to maintain capacity and services during a second wave as well as continuing scheduled surgeries to reduce wait lists and backlogs.
About St. Joseph’s Home Care
Since 1921, St. Joseph’s Home Care has provided high quality, values-based home and community services in a spirit of compassion and dedication. We have evolved from a nursing agency to offering a much broader range of services, and our steadfast commitment to delivering exemplary client-focused care to the Hamilton community continues.
About St. Joseph’s Health System
St. Joseph’s Health System (SJHS) is one of the largest healthcare organizations in Canada, and is the only system in Ontario delivering a full continuum of health care services. SJHS is a globally recognized leader for innovation in models of patient-centred integrated care. SJHS has a unique partnership with Niagara Health to leverage each organization’s strengths to bring better care to the people in the communities we serve.
About Niagara Health:
Niagara Health is a regional healthcare provider with multiple sites and a growing network of virtual and community-based services. We provide a wide range of inpatient and outpatient services to more than 450,000 residents across Niagara, including Acute Care, Cancer Care, Cardiac Care, Complex Care, Emergency and Urgent Care, Kidney Care, Long-Term Care, Mental Health and Addictions, Stroke Care and Surgical Care.
About St. Joseph’s Healthcare Hamilton
As a premier academic and research healthcare organization, St. Joseph’s Healthcare Hamilton is committed to making a difference in people’s lives and creating a lasting future for our community through integrated health services and internationally recognized programs. Our threefold mission is to provide dynamic research, revolutionary methods in health sciences education and the highest standard of clinical care in a spirit of compassion, innovation and commitment.
For More Information:
Patrick Moore
Senior Public Affairs Specialist, St. Joseph’s Health System
M: 905.870.1293 | E: pmoore@stjoes.ca
Steven Gallagher
Communications Specialist, Niagara Health
P: 289-696-6767 | E: Steven.Gallagher@niagarahealth.on.ca
In 1890, our founders, the Sisters of St. Joseph of Hamilton opened a 25-bed general hospital. Over the last 130 years, we’ve established our reputation as a leading academic, multi-site hospital. In June 2020, we are celebrating 130 years of caring for our community and beyond.
Our pioneering spirit at St. Joseph’s Healthcare Hamilton began in 1852 when the Sisters of St. Joseph of Hamilton arrived to care for those most in need, a commitment that only intensified with the outbreak of cholera. Compassionate care for all is the Sisters’ legacy when they opened the doors of our hospital 130 years ago. This legacy continues to be infused in the foundation of the work we do each day at St. Joe’s, especially as we face the current COVID-19 pandemic together.
Over the last 130 years, each one of our employees, physicians, learners and volunteers have been committed to excellence and dedicated to discovery. In honour of all you have built together and all of the lives you have touched, we’re sharing some St. Joe’s ‘Then and Now’ photo moments.
Click and drag the bar in the centre of the photos to reveal the ‘Then & Now’ photos.
Pictured Above
Left photo: Sr. Euphrasia (left) and Sr. Angela (right)
Right photo: David Czaplinski, Registered Nurse, Waterfall 1 (left) with a laptop on wheels and Basma Ghwila, Patient Clerk Unit Clerk, Waterfall 1 (right) using a smart screen as a computer monitor
Pictured Above:
Top Photo: Sr. Jane (right) with patient in dialysis in the 80’s.
Bottom Photo: Randy Orlicki, Registered Nurse in our dialysis unit.
Pictured Above
Left photo: Sr. Mary Austin Reding in the busy nursery. Sr. Mary served in Maternity at St. Joe’s from 1957 – 1961.
Right photo: Justine Brown, Registered Nurse, Special Care Nursery.
Pictured above
Top photo: Sr. Teresita McInally, General Superior, 1990.
Bottom photo: Jennifer Olarte-Godoy, Nurse Educator, Mood Disorders, F1 and Nursing Resource Team
Thank you for 130 years of Leading, Learning, Building and Caring.
HAMILTON, ON (May 21, 2020) – Scientists at The Research Institute of St. Joe’s Hamilton have developed entirely novel COVID-19 testing methods, which will allow for a significant increase in testing capacity across the province.
The new methods are being implemented in the Hamilton Regional Laboratory Medicine Program (HRLMP) – a partnership between St. Joseph’s Healthcare Hamilton and Hamilton Health Sciences – which is responsible for conducting clinical COVID-19 testing for the region. Currently, the HRLMP clinical testing capacity is 800 samples per day. With these advancements in place, scientists are aiming to test up to 6,000 samples daily.
Dr. David Bulir and Dr. Marek Smieja, infectious disease physician-researchers from St. Joe’s Disease Diagnostics and Development (D3) Group, predicted the need for an alternative supply of testing materials in January.
“In the face of global shortages, we’ve had to secure a new supply of all the materials required for COVID-19 testing, as well as invent some components that enable mass testing,” said Dr. Gail Martin, Executive Director of The Research Institute of St. Joe’s Hamilton. “St. Joe’s has effectively rebuilt and secured an entire supply chain, one that is urgently needed to manage the shortage of testing supplies.”
While some materials have been sourced and validated from new suppliers, such as flocked swabs and specimen tubes, other materials, including the new transport medium, are entirely novel. Dr. David Bulir developed the new transport medium and an enhanced test for COVID-19 at St. Joe’s research laboratory.
One of the key benefits of using these new testing materials with Dr. Bulir’s newly developed COVID-19 test is the ability to pool specimens. Specimen pooling can enable labs to increase their testing capacity up to fourfold, and potentially more. Since most tests produce negative results, only pools that come back with positive results will need to be further examined.
Building up the province’s stockpile of testing supplies and its capacity to perform rapid testing are vital as municipalities gradually lift lockdown restrictions.
“We’re working with the province to ensure we can rapidly develop ways to provide these new materials to other labs,” said Dr. Martin. “This is a Made-in-Ontario solution to a critical global shortage.”
This project will have a significant impact on the increased testing that will be needed to emerge from COVID-19, the value of which has been demonstrated through the Surveillance Pilot Project, launched in collaboration with St. Joseph’s Health System. That project aimed to detect the spread of COVID-19 and determine the most effective testing strategies in long-term care and congregate settings.
Development of these innovative testing methods could not have been possible without the support and funding from the Juravinski Research Institute, the Ontario COVID-19 Rapid Research Fund, St. Joseph’s Health System, and The Research Institute of St. Joe’s Hamilton.
Premier Doug Ford announced the Ontario COVID-19 Rapid Research Fund projects at a press conference Thursday afternoon, expressing his enthusiasm for the St. Joe’s project.
Background Info:
Shortage of testing supplies
- Due to factory closures in Italy where the gold-standard flocked swabs and transport media are produced, as well as stockpiles that were not maintained at pandemic-level quantities by manufacturers, standard testing supplies are scarce.
- St. Joe’s researchers designed a new supply chain to address this issue across Ontario
Specimen pooling
- Instead of running each specimen through its own test, specimens can be combined into a single test to increase throughput.
- Since most tests are expected to have negative results, pooling allows for massive increases in concurrent testing. Specimens pools that come back positive can be further tested individually.
- Pooling will allow many more tests to be performed in the same timeframe
Deployment of robotic liquid handling technology
- Using robotics in the laboratory reduces risk to lab technicians, while increasing the speed and the number of concurrent tests that can be run
New transport medium
- A transport medium is the liquid in the specimen tube that maintains the integrity of the sample while it is transported to the lab.
- Unlike many transport media that keep the virus intact before testing, St. Joe’s new transport medium breaks down the virus, effectively killing it.
- The new transport medium works well with Dr. Bulir’s robust COVID-19 test. This new medium reduces biological risk to the scientists conducting the tests and enables increased testing capacity.
Published: Thu., May 14, 2020
Forty-one days, at least six tests and two negative results.
That’s what it took for Helen Keene to see the light of day beyond the COVID-19 unit of St. Joseph’s Hospital.
On Wednesday, she was finally discharged to fanfare.
Lining the hall, nurses, doctors, cleaners and other hospital staff clapped as registered nurse Tanirose Guiao pushed the 71-year-old’s wheelchair out the doors.
“My heart exploded,” said Keene. “I was so overwhelmed with the kindness and generosity. That was a gift.”
Keene was admitted to hospital in early April when she became one of the first residents infected with the respiratory virus at Cardinal Retirement Residence.
The Herkimer Street institution has been home to one of the worst outbreaks of the virus in Hamilton. There were 65 cases — 47 residents and 18 staff — before the outbreak was declared over May 3.
When Keene first came down with the virus, she was having trouble breathing, she had a fever and her white blood cell count had dipped.
Due to her medical history, which includes open heart surgery and stent, Keene was put on a heart monitor. She also developed a “horrendous” cough.
“It was so bad my rib cage was bruised and sore,” she said. “I couldn’t even touch my chest, I was in so much pain. It hurt to breathe.”
But, Keene still counts her lucky stars that she never ended up on a ventilator — a story she became far too familiar with hearing in the hospital.
“I was one of the blessed ones,” she said. “I was thankful for that every day.”
Having been under close watch by staff, Keene said she now considers those who cared for her to be her “extended family.” Guiao, a 23-year-old nurse from Burlington, was with her through the entire journey.
The pair got to know one another between waves at the windows and chats while Guiao was checking in on her. Guiao knew Keene was grieving the loss of her husband, Michael, who died two years ago and that the song “I’ll See You Again” by Westlife kept her grounded.
Last week, following a negative result, Keene tested positive again. Lying in bed, feeling depressed and missing Michael, Keene suddenly heard the tune over the intercom, dedicated to her by the team.
“It made the … stay possible to tolerate,” she said. “It was unbelievable what they did for me.”
But on Wednesday, that news shifted.
Guiao was able to deliver Keene the results she had been waiting for — she had tested negative for the second time in 24 hours and she was going home.
“We were screaming and yelling and we high-fived each other,” said Guiao. “It was such a joy.”
Even if it had been positive once again, Keene’s resilience in the hospital was “inspiring,” she added.
“(Helen) never gave up and she always had a positive attitude,” said Guiao. “It was a pleasure caring for her … she’s a fighter.”
Having “conquered” the virus, Keene is hopeful that people will continue to follow physical-distancing measures, live day by day and avoid feeling resentful for the time they may miss with their loved ones.
In her own condition, Keene realizes she could have been one of the “unlucky ones.” As of Thursday, the virus had claimed the lives of 25 people in Hamilton.
“You don’t know what to expect, and no one can tell you what to expect,” she said. “It comes back down to who you are and what you have to offer.”
Fallon Hewitt is a Hamilton-based reporter at The Spectator. Reach her via email: fhewitt@thespec.com
BY DON MITCHELL GLOBAL NEWS
Two well-known philanthropists are set to give Hamilton health researchers a $3.3-million boost to help fund urgent research projects connected to the COVID-19 pandemic and mental health.
In a letter to the community, Charles and Margaret Juravinski say they are donating funds to free everyone from the “terrible virus,” and allow the public to “live and move about without fear of spreading or picking it up.”
“Like everyone, we are deeply troubled by the fearsome threat of COVID-19, which has truly changed the world in just a few months,” the couple said in their letter.
“We are concerned not for ourselves, but for the people around us: our friends and family, our neighbours near and far, the people who work in our community’s grocery stores, restaurants and hospitals and the kids who should be out playing in our schoolyards.”
The money is an advance on a pledge made in May when the couple promised to divide their $100-million estate between Hamilton Health Sciences, McMaster University and St. Joseph’s Healthcare Hamilton, a gift they say would generate up to $5 million annually for the three agencies under the banner of the Juravinski Research Institute.
Charles, 90, and Margaret, 88, known for endowments with a number of projects connected to the city, McMaster University, and healthcare, compare the COVID-19 pandemic to a number of “frightening problems” they experienced during their lifetime including the Great Depression, the Second World War and the scourge of polio.
“Our wish is that it may inspire hope,” the couple said of the donation, “We hope it will produce results that benefit people immediately. We urge others to find ways to give what they can.”
In a joint statement, Hamilton Health Sciences, McMaster University and St. Joseph’s Healthcare Hamilton say the funding will support eight collaborative research projects which include:
- A study on the effectiveness of N95 respirators or medical masks
- A three-part study on the impact of the pandemic on hospital emergency departments and staff
- speed up of diagnostic testing protocols for viral pathogens responsible for the COVID-19 using robotics
- An age-related study of 50,000 people ages 45 to 85 to close in on factors that appear to protect against or increase the risk of developing symptoms connected to COVID-19
- COVID-19 repository for storing human biological samples
The money is also earmarked for three mental health projects including a study on the impact of substance use in relation to the brain development of young adults, technology to identify brain anomalies following a mild traumatic brain injury, and AI technologies offering data on potential treatments to aid youth mental health.
St. Joseph’s says use of virtual visit tech has increased 450 per cent
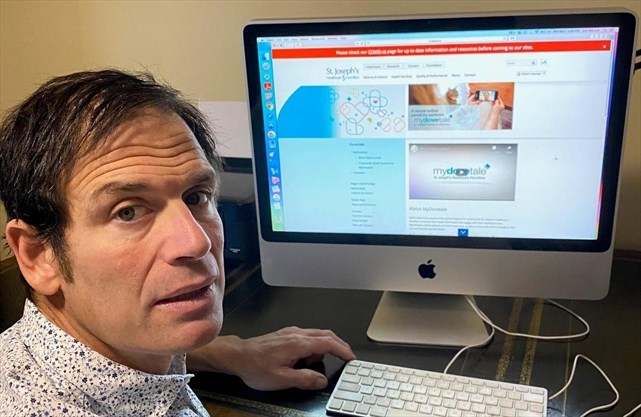
Rob DeLuca, a bodybuilder with stage-four lung cancer and pulmonary hypertension, uses St. Joseph’s Healthcare Hamilton’s digital patient portal, MyDovetale, from his Ancaster home.
Apr 01, 2020 by Sebastian Bron Hamilton Spectator
For Rob DeLuca, an ordinary trip to the doctor’s office often feels like tiptoeing through a room filled with trip wires.
The bodybuilder with stage-four lung cancer and pulmonary hypertension is acutely vulnerable to commonly transmitted germs. Touchscreen parking posts, arm rests on chairs, door handles, washrooms: they’re all akin to booby traps that could trigger an infection and kick his immune system into overdrive.
But that’s changed as the outbreak of COVID-19 has forced health-care providers to embrace physical distancing and modify their outpatient care services.
DeLuca was one of more than 1,000 at-risk St. Joseph’s Healthcare Hamilton (SJHH) patients to have received virtual care in March, chatting with doctors and getting condition updates from the comfort of their own homes.
“It’s made a big difference, especially since we’ve always had to be ultra-mindful when going to the doctor and now that’s been (amplified) with the virus,” said DeLuca, who meets with a respirologist every three months.
“There’s no travel, getting through several doors, touching many surfaces. There’s more time to discuss with (the doctor) and my wife can sit comfortably on the couch taking detailed notes.”
SJHH has seen an approximately 450 per cent increase in virtual-care volume since its personalized, digital patient portal, MyDovetale, was streamlined last month to cope with the number of people who wouldn’t be able to access on-site services.
Tara Coxon, chief information officer, said SJHH has seen an increase from 100 patients before the crisis — most of them mental health — to about 5,000 now across 19 clinics.
“Emergency visits to clinics are still operating, but for the part we’ve had every service go digital,” she said.
The user-friendly system has given doctors a reliable means of adapting their care to the current limits of the health crisis. For patients whose technical capacity is underdeveloped, like seniors, the health centre has a team of nurses and researches help get them on board.
“Physical distancing is critically important during COVID-19, and this has helped us go on with business as usual,” said Dr. Nathan Hambly, a respirologist at SJHH’s Firestone Clinic and DeLuca’s doctor.
The Firestone Clinic has about 700 patients with complex respiratory diseases, a majority of which boast survival rates of around three to five years.
With appointments typically scheduled months ahead of time, Hamby said the virtual portal — and in particular seeing his patients over a screen — has proven imperative in offering patients consistent, accurate care during the health crisis.
“One might say that a telephone would be just as good in these situations, but it isn’t. By looking at a patient, you’re able to ask questions and see their breathing and how hard it is for them to breath in real time,” he said.
Sebastian Bron is a Hamilton-based reporter at the Spectator. Reach him via email: sbron@thespec.com








